
Understanding Bedwetting (Nocturnal Enuresis)
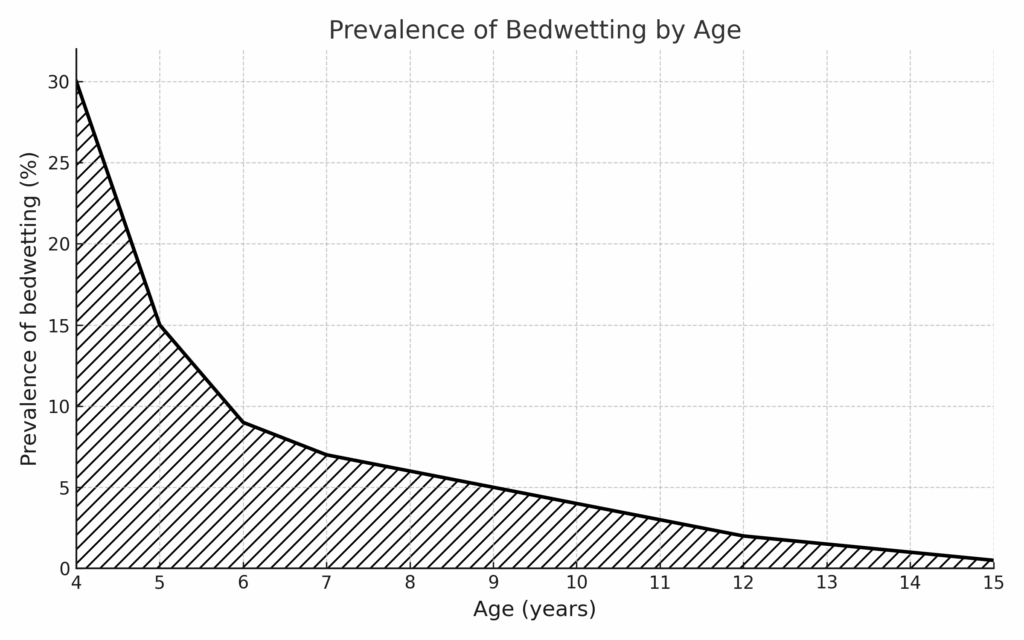
Night-time bladder control is not expected until a child reaches the age of 5 to 7. At 4 years old, nearly one in three children wets the bed, but this decreases to about one in ten by age 6. Bedwetting (or nocturnal enuresis) refers to involuntary urination during sleep. It presents in different forms for example some children may urinate several times a night, while others release a large volume of urine near dawn. In all cases, the key feature is the child’s inability to wake in response to a full bladder (Chart adapted from the Royal Children’s Hospital Melbourne).
Western Medicine Perspective
From a Western clinical perspective, most cases of bedwetting are not due to underlying medical or emotional disorders. However, persistent bedwetting can significantly affect a child’s confidence and social life, particularly around sleepovers and school camps.
Common contributing factors include:
-
Delayed development of bladder control
-
Deep sleep patterns where the urge to urinate doesn’t wake the child
-
A family history of enuresis (genetic predisposition)
-
In some cases, increased night-time urine production (nocturnal polyuria)
Treatment is generally recommended for children over 6 years old if bedwetting is frequent or distressing.
Management strategies may include:
-
Lifestyle changes (e.g., reducing fluid intake before bedtime)
-
Scheduled night-time toileting
-
Bedwetting alarms
-
Medications
The success of any treatment depends on consistency, parental support, and a non-punitive approach. If the child also experiences daytime urinary symptoms, further medical evaluation is necessary.
Recommended resources from Royal Children Hospital:
Traditional Chinese Medicine Perspective
In Traditional Chinese Medicine, bedwetting is understood as a manifestation of underlying imbalances in the body’s organ systems, particularly those involved in fluid regulation and energy (Qi) flow. According to Traditional Chinese Medicine theory:
The Kidneys play a central role in regulating the bladder’s ability to retain urine. When Kidney Qi is weak or there is a deficiency in Kidney Yang, the body may struggle to maintain control during sleep, resulting in bedwetting.
The Spleen is essential for the transformation and transportation of fluids. Children with Spleen Qi deficiency may also exhibit digestive symptoms such as bloating, reduced appetite, or loose stools, alongside nocturnal enuresis.
The Lung assist in directing Qi and fluids downward. Children with Lung patterns can also present respiratory conditions like asthma, recurrent colds, or allergies, alongside nocturnal enuresis. Structural issues (e.g deviated septum) can further disrupt the communication between the Lungs and Kidneys, impacting body’s ability to regulate urination.
Children who are emotionally sensitive or constitutionally “cold” may be more susceptible to enuresis. Cold weather, poor sleep, or fatigue can aggravate the symptoms, especially in children with Kidney Yang deficiency. Of course, chronic bedwetting itself can become a source of emotional distress, reinforcing a cycle of anxiety, shame, and further dysfunction. In such cases, the psychological burden worsens the imbalance, which may deepen the condition if left unaddressed.
Treatment in TCM is highly individualised and holistic, focusing on strengthening organ systems, improving circulation, and calming the nervous system. Common strategies include:
Japanese paediatric acupuncture, needle-free
Japanese acupuncture, known for its delicate technique and ultra-fine needles
Moxibustion, a warming therapy that applies heat to specific acupuncture points (e.g. lower abdomen and sacral area)
Chinese acupuncture and herbal medicine, prescribed according to the child’s pattern diagnosis
Lifestyle guidance, such as keeping the abdomen and feet warm, reducing cold/raw food intake, and maintaining a regular sleep routine
Parents are also taught gentle acupressure and home moxa routines to reinforce clinic-based treatments and build the child’s confidence and sense of control.
By combining modern clinical tools with traditional wisdom, families can take a more comprehensive and supportive approach to care. Starting treatment early, ideally before stress-inducing events like school camps, can make a significant difference. Nocturnal enuresis deserves patience, empathy, and understanding from both Eastern and Western medical perspectives.
get in touch
Have any questions about Acupuncture and Moxibustion treatments? Sara is available to discuss your health concerns and treatment options.
Copyright © 2023- 2026 Acupuncture Moxa Melbourne – All Rights Reserved.
